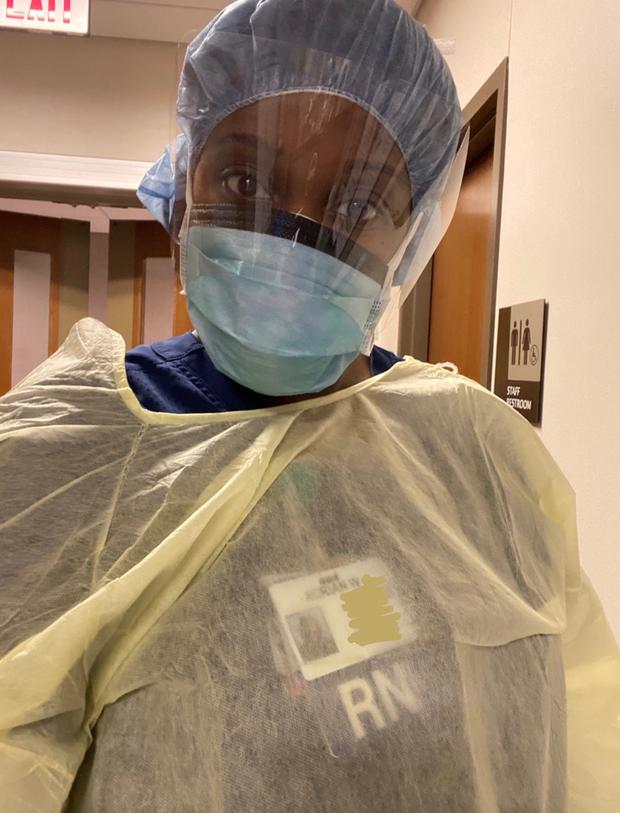
On The Frontlines: A Look Inside The Covid-19 Pandemic From 2 Detroit Nurses
DETROIT, Mich. (CBS DETROIT) - Michigan confirmed its first two coronavirus cases on March 10 and since then, the state has reported more than 29,000 confirmed cases and over 2,000 deaths as of April 16; all while first responders and essential workers continue to provide support for their communities, showing us we are in this together.
Two Detroit nurses spoke with CBS 62 Digital Producer Bria Brown about their experience on the frontlines during the pandemic. AaLona Robinson made a split decision to leave her family in Detroit and serve in New York — where at the time, confirmed cases were over 15,000 and just over *1,000 in Michigan — while Adrian Williams has recovered after testing positive for COVID-19 and has since returned back to work.
Here are their stories.
AaLona R., 32, has been in healthcare for 15 years. When she learned about New York's positive cases, she made her decision at 1 a.m. on March 22 and immediately booked a flight. She was in NY by 8 a.m. ready to work.
Bria Brown: What made you want to leave Detroit and travel to New York and help, when Michigan had confirmed cases?
AaLona R.: I had been been following Governor (Andrew) Cuomo because he's been really transparent. I was watching him on the news and he was explaining that it was 15,000 in New York. Now looking back I feel guilty almost every day about not being at home because it's spread so much in my own hometown, but I've already made a commitment to be (in New York).
BB: Are you at one specific hospital or do you go to multiple hospitals in New York?
AR: The company that I work for assigns us to a specific hospital. Where I go in that hospital changes, but usually I'm on the same unit because the unit that I work on, they opened for COVID. It wasn't even a unit.
BB: Do you think you being on the frontlines here or in New York has been more effective during this pandemic?
AR: I feel like I can be more effective here (New York) because it's truly like laser focus on my work here. If I'm home, I'd be worried about my son and worry about the family and I probably would end up taking time off if I was home because I don't want to infect my family. I would be isolated from them anyway and I think that would be harder for me to be, you know, two miles away from my family and not being able to see them because I'm going to work. It would be harder for me to choose work over my family if I was (home).
BB: You are very transparent on your social media page. Have you received any backlash for documenting your journey in New York from people in Michigan?
AR: Very interesting question. On my social (media), I haven't received any backlash about it or any negativity because I think that I started so early. I was already out here before it really started hitting Detroit, so people understood that it wasn't like, it got bad in Detroit and then I jumped in. I was already out here so, it was already in people's brains that I would be in New York. So I don't think there was negativity related to that.
BB: How long was your assignment supposed to be in New York?
AR: It was supposed to be two to three weeks, 14 to 21 days straight. Every day, 12 hour shifts. I did take a mental health day, I was assaulted by a COVID positive patient, he was angry. Most patients are, you know, they're scared. He assaulted me. He apologized and explained to me he was scared and it's not like that made it OK but, you know, that did happen. I took a day off and that's when I went home for that one day.
BB: How do you self care?
We're allowed one day, if you make it to 14 days — which a lot of people haven't. I would say about 30 percent of nurses don't make it 14 days. A lot of people that I started with on assignment are not here — so, once you make it to 14 days you get one day off. On my 14th day I took a day off. I bought myself some flowers, I keep fresh flowers here and I make sure to talk to my son and family everyday and I listen to music.
BB: Other than self-quarantine how are you making sure you and your family are protected?
AR: I'm very very OCD about my PPE (personal protective equipment). I don't walk past the hand sanitizer machine without using it. I wash my hands like 50 million times a day and shower at least twice a day. I'm staying away from my family, it's easy to do when I'm not in the same city. Even when I went home, I talked to my grandmother through her screen door. I talked to my son through a screen door, there was no hugging (or) embracing. It's very difficult and even when I went home and saw him and my grandmother, and the conditions in which I (had) to interact with them — it made me want to come back here and fight this.
Adrian W., 26, developed symptoms at work and was later tested for COVID-19. Her results were positive and she was self-quarantined.
Bria Brown: What were your symptoms?
Adrian W.: I had a fever of 105 (degrees) for six days. I had severe body aches for six days and on the sixth day, I developed shortness of breath and a cough, that's when I had to go to the hospital. I have asthma so I couldn't really breathe. My symptoms lasted for 14 days.
BB: How did self-quarantine affect your mental health?
AW: I was sad because I had to be by myself. Nobody can come take care of you. It's hard to be by yourself for a full 14 days. Yes, people call and text, but you really don't have any energy.
BB: How do you feel when you see people who aren't adhering to Governor Gretchen Whitmer's executive order?
AW: It frustrates me because I risk my life and I got sick. We have multiple people, so (that means) multiple patients, it was just frustrating to (nurses) because supplies were scarce making it difficult to care for people. So for (people) to disrespect it, means you're willing to get sick and add to the patient load, when you could be healthy and just stay at home.
BB: With your nursing experience did you feel you had an advantage to overcome the coronavirus?
AW: Even though I am a nurse, the nurse in me didn't kick in all the time because I was so tired. I didn't know what to do. I just needed to survive and try to make it through it. This illness is so new and me being young, people were like, 'Did you feel like you had pneumonia,' but I've never had pneumonia before. I've had the flu before, and it is worse than the flu.
BB: Did returning to work cause you anxiety?
AW: Yes and no. Not about getting coronavirus again because I beat it, and the nurse inside of me knew that I developed antibodies, so it would be a small chance for me to get it again. What made me nervous was the patient load and experiencing deaths. Of course I'm very thankful to have survived it, but it just sucks having to talk to other family members because a lot of people died from this, and I could have potentially died. It makes me anxious every day to go to work because I'm not looking forward to seeing people die from the same thing I survived.
BB: Do you feel this pandemic has detoured people from wanting to become first responders.
AW: No. I think there's like a lot of people I know who are in (nursing) school right now who will be graduating and they're eager to come in and help the workforce. A lot of people are fueled by adrenaline, or like challenges so because we're going through this, this is a challenge for the whole entire world. I feel like they want to be a part of it. There's a lot of good people who want to change the world.
BB: Other than what the public has already been told, can you think of anything else that we can do to help to flatten the curve?
AW: Definitely. Washing your hands after everything and making sure you wipe down everything, including stuff you may not realize like your steering wheel, your car door handles and making sure you don't wear gloves out in public. As a healthcare provider it's frustrating because we use gloves to provide patient care and lessen the risk of cross contamination. We wash our hands before we put on gloves and after providing patient care, we dispose of the gloves and wash our hands again. Unlike in a public setting gloves are being used improperly. I see people with gloves on talking on the phone, touching boxes, touching the buggies, which could lead to further cross contamination. Gloves carry more germs than your hands because it's a better surface to keep germs on, so please remember to wash your hands and continue to practice social distancing.
*More than 1,000 coronavirus cases were confirmed in Michigan on March 22 according to the Michigan Department of Health and Human Services.
© 2020 CBS Broadcasting Inc. All Rights Reserved. This material may not be published, broadcast, rewritten, or redistributed.